To Floss Or Not To Floss - Your mouth and your heart.
- Lola Oni

- Feb 8, 2021
- 3 min read
ORAL HYGIENE
We talk, we eat, we drink, we sing, we laugh, we smile – these are activities that we do everyday without giving it a thought. Doing these with confidence depends greatly on whether the mouth - ‘our window to the world’ as termed by some, is in a healthy condition.
Besides the above, one thing that is not so apparent is how poor oral health contributes to other long term systemic conditions. These are 3 oral conditions which have been linked to long term conditions:
Dental caries – is a common bacterial condition, caused by lactic acid formed from bacteria fermentation of certain carbohydrates eroding the tooth enamel. You may begin to experience sensitivity, especially with hot, cold or sweet foods, black or brown discolouration and holes or pits in the teeth.
Gingivitis – is redness, swelling, puffiness and bleeding of the gum. Bleeding may happen with or without pain. This is an inflammatory condition caused by bacterial infection.
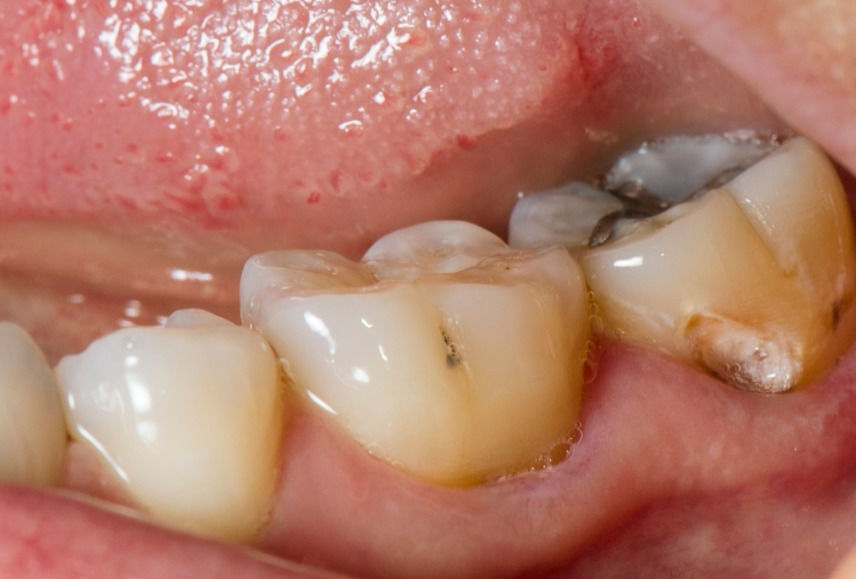
Periodontitis – when gingivitis is left untreated it progresses to periodontitis, where the soft tissue begins to come away from the teeth. There is also loss of connective tissue and bone and eventually teeth loss. The structural change of the gum around the tooth gives room for pathogenic bacteria to flourish. That triggers an immune response and further damage to the surrounding tissues.

Physical loss of teeth can also affect ability to chew, eat nourishing meals, talk, sing, smile, laugh and your quality of life.
As said earlier, some of the systemic conditions that have been linked to oral health are;
-Cardiovascular disease – Of course there are many other obvious causes of heart disease. On the issue of oral hygiene, evidence is growing on the connection. Chronic inflammation, deep seated infection and damage to vascular structures are the ways that have been identified to be liked to heart health.
-Pulmonary disease – such as pneumonia, COPD (chronic obstructive pulmonary disease) and bronchitis involve infiltration of pathogens from the oral cavity to the respiratory tract.
-Diabetes – it has been noted that high levels of blood glucose for prolonged periods affects oral health. At the same time, severe periodontitis impacts control of blood sugar due to the persistent inflammatory state of the body.
Other conditions which are being investigated for their causal relationship to oral health are osteoporosis and chronic kidney disease.
You will never imagine that there could be a connection between your mouth and these conditions. And you never know what other connections to inflammatory illnesses that are yet to be discovered.
Prevention is the best approach.
1. Make regular visits to your dentist. You do not have to experience symptoms to see your dentist.
2. Follow the recommended advice of brushing twice daily, keeping to the motions as shown by your dentist.
3. Flossing is considered unnecessary by many. Some claim there isn’t enough evidence to show that it is of benefit. Well, if we just use logical reasoning, that you brush your teeth and tongue to keep your mouth clean, fresh and reduce bacterial load, it is also true that the brush cannot get in-between the teeth to clean out left over foods. This is where flossing comes in handy.
Note that you need to be shown how to floss effectively by your dentist, so that you are not causing damage to your gum.
4. I believe it is a good habit to rinse out your mouth with water after eating, and if not convenient, then make sure to drink water. In doing that, you are reducing the bacteria load in your mouth and the consequent corrosive effects of products from breakdown of food.
Good oral health can reduce susceptibility to ill-health.




Comments